This website uses cookies so that we can provide you with the best user experience possible. Cookie information is stored in your browser and performs functions such as recognising you when you return to our website and helping our team to understand which sections of the website you find most interesting and useful.
We are experts for
hoof surgery
hoof cancer
equine canker
Equine canker has nothing to do with thrush!
Equine canker is a growth process, thrush is a decay process!
Equine canker has nothing to do with classical cancer.
There are neither metastases nor melanomas or anything else.
Therefore, the term “hoof cancer” is actually wrong or misleading. But the good news is: if the disease is treated professionally, the chances of recovery are very good.
However, it is important to note that successful equine canker treatment is teamwork – between the veterinarian, farrier and horse owner.
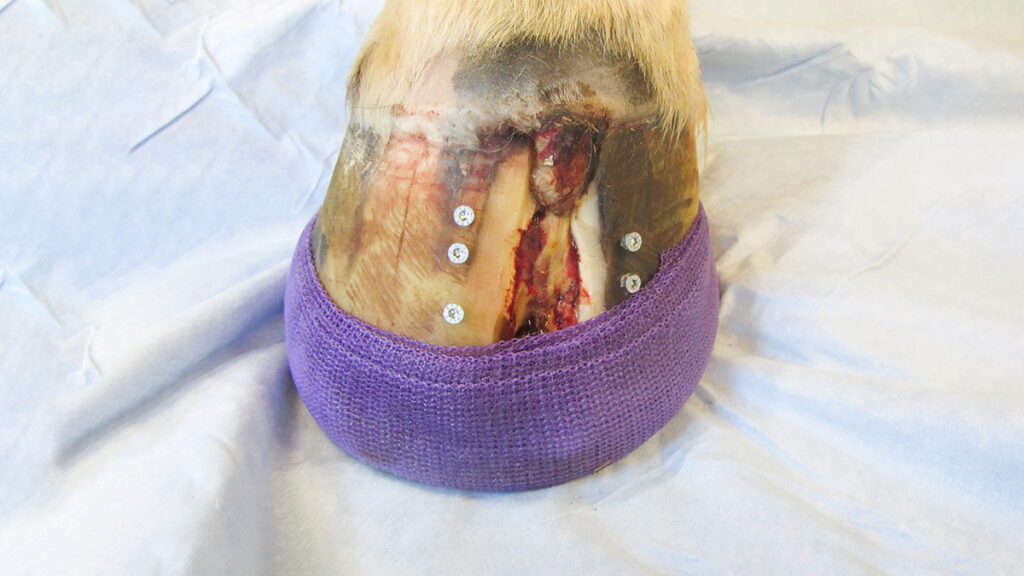
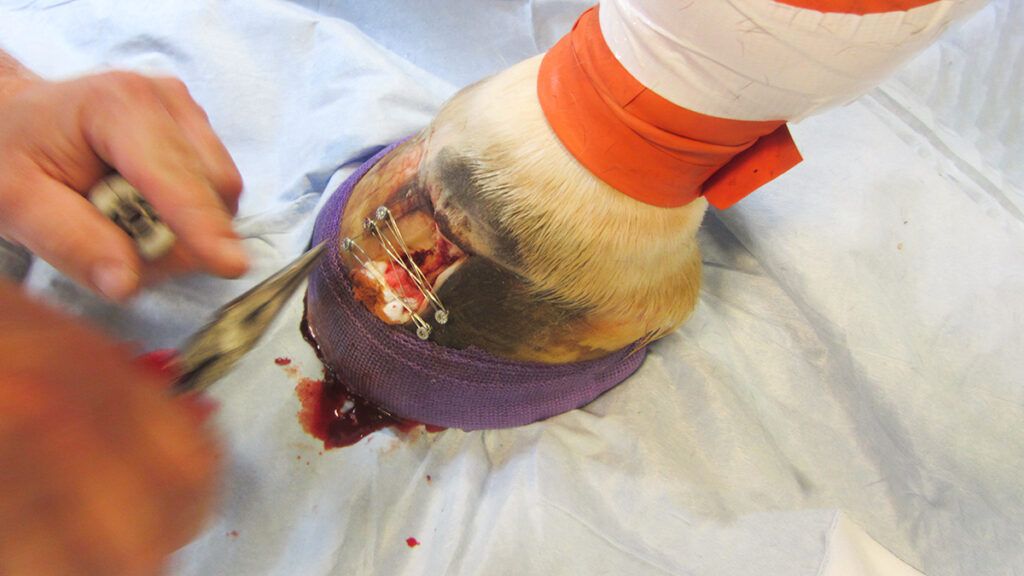
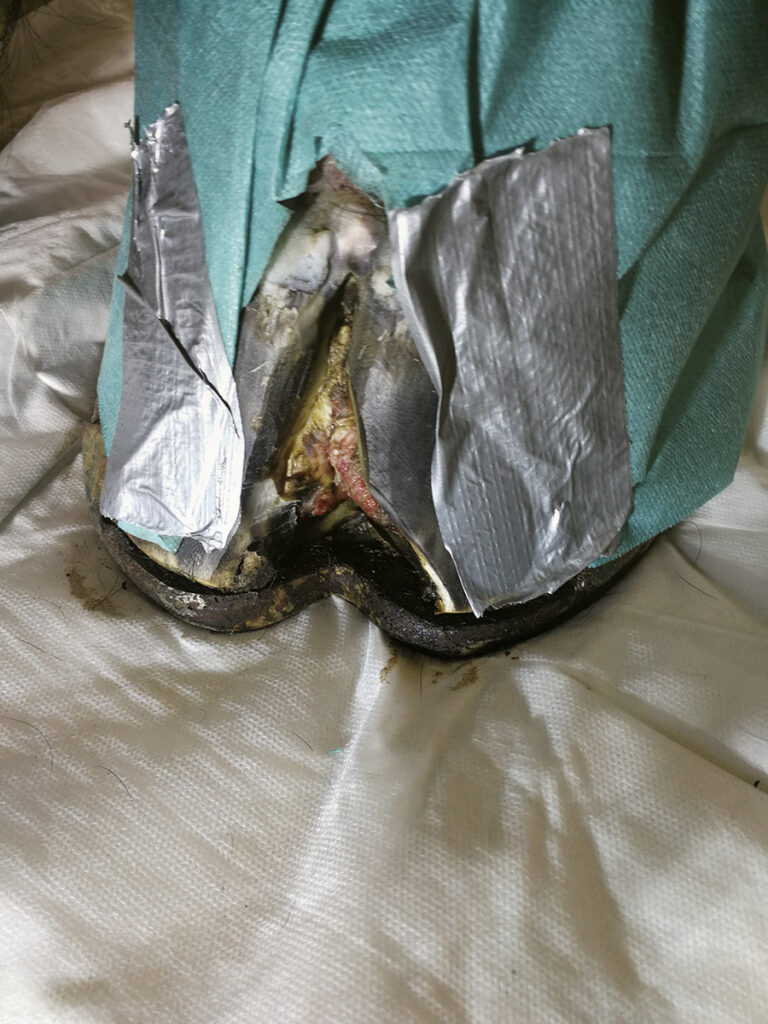
Equine canker is often only detected after it has clearly spread. Therefore, only radical surgery can be considered. The affected areas on and under the hoof must be radically surgically removed. Sometimes, unfortunately, the hoof pads and corner strut walls have to be removed as well. Merbromin and Lotagen solution has proven to be a good wound care and also later to accelerate healing. The classic horse shoe as well as plaster bandages are well suited after surgery to ensure a strong pressure bandage. The pressure bandage is extremely important for healing, because only under pressure can a targeted keratinisation be attempted. Often the horses are free of pain and lameness only a few days after the operation.
Depending on the severity of the disease, patients need 8 –16 weeks to recover. If the equine canker is detected early, a mixture of sclerosing agents has proven to be effective. Applied daily, an operation has sometimes become superfluous.
In principle, we try to work as minimally invasive as possible.
Markus Raabe has treated more than 700 equine canker patients so far. The customers come to us from all continents.
Keratoma
Most often, keratoma occurs in the hoof wall area. It probably develops as a result of an injury or inflammation in the area of the coronet. This causes a “scar” in the area of the horn-producing cells, which then produces the keratoma. In some cases, keratoma can also occur following a hoof abscess.
Keratoma can usually be recognised at the wall edge. On the one hand, the keratoma can press on the corium and on the coffin bone and thus cause inflammation of the corium and/or coffin bone; on the other hand, the keratoma consists of inferior and poorly structured horn, which decays prematurely and thus does not provide effective protection against fungi and bacteria. This results in more frequent infections such as hoof abscesses.
Radiographically, one typically sees a well-demarcated bone dissolution in the coffin bone in the area of the keratoma. Diagnostic anaesthesia of the nerves can be used to localise the lameness reliably to the hoof and subsequent treatment can be carried out painlessly.
The veterinarian performs diagnostic anaesthesia to desensitise the hoof. The entire keratoma must be surgically removed by the farrier so that normal horn can be produced again.
After the keratoma has been removed, the hoof is stabilised with a special shoe.
hoof abscess
A hoof abscess is a collection of pus in the corium. It usually develops from small infectious inflammations of the corium. Bacteria must therefore be involved. If only superficial parts of the corium are affected, the pus is usually thin and possibly black due to the melting of pigmented cells. If deeper layers are involved, the secretion is usually thicker and more yellow. The older the abscess, the more brownish the colour of the pus.
A hoof ulcer is usually not difficult to recognise. The inflammation causes pain to the horse as soon as the pus starts to press on the neighbouring sclera sections. Then the typical severe, often sudden lameness can be observed. Affected animals often try to relieve the leg. Due to the inflammation of the hoof corium, the hoof usually feels warm. A throbbing may be felt at the back of the fetlock head, the pulsation of the toe artery. If the inflammation is very severe and painful, the horse may even develop a fever or refuse to eat.
If a hoof abscess is suspected, the shoe must be removed and the abscess searched for with hoof forceps. The abscess is cut open, but the hole must not be too large on the inside so that the corium does not protrude. The hole must be widened to a funnel shape on the outside so that the canal does not close again.
Then an dressing with Rivanol or similar is applied for two days. If the wound does not need to be re-cut, dry dressings are applied until the irritation of the corium has subsided, i.e. the wound is dry and the horse is no longer lame. After the abscess has healed, a smooth connection must be made between the hoof corium and the horn edge of the hole, otherwise a double sole can easily form.
Some horses do not walk completely straight again until they have been shod. It is also possible that the corium will continue to secrete some moisture for some time. Therefore, the hole must never be plugged even after healing! As the new horn is very sensitive at first, the horse should be given a shock-absorbing insert for a shoeing period.
With every hoof abscess, the question of tetanus protection is important!
Hoof wall cracks
Hoof wall cracks are vertical separations in the area of the hoof wall in longitudinal direction. A distinction is made according to location and depth. A deep crack from the coronet band to the bearing edge is the through-going wall crack. Often the cracks extend to the hem band of the growth zone of the wall. If this is injured, these cracks can bleed constantly. But don’t panic, even these cracks are treatable in most cases. Deep wall cracks always require treatment, as they cause instability of the horn capsule and lead to changes in hoof shape. Horses with wall cracks often have pain due to bruising and overloading of the sensitive, highly innervated wall dermis, which is often accompanied by lameness.
Another problem is putrefaction processes in the crack, caused by bacteria that already colonise the crack in symbiosis with the formation of the crack. The crack provides an ideal environment for these bacteria to multiply. These putrefaction processes often lead to further complications, e.g. infections with abscess formation.